- 18th April 2026
Table of Contents
- Age does not cause diabetes directly, but it slowly reduces your body’s ability to handle sugar
- Does Age Directly Increase Blood Sugar?
- Decline in Insulin Sensitivity
- Loss of Muscle Mass (Sarcopenia)
- Increase in Abdominal Fat
- Changes in Hormonal Regulation
- Reduced Physical Activity and Its Impact
- Slower Metabolic Rate
- Impact of Sleep and Stress
- Medication and Comorbid Conditions
- Why Post-Meal Sugar Becomes More Important With Age
- The Cumulative Effect Over Time
- What Can You Do to Maintain Better Sugar Control With Age?
- 1. Preserve and Build Muscle Mass
- 2. Focus on Meal Composition
- 3. Stay Consistent With Physical Activity
- 4. Improve Sleep Quality
- 5. Monitor More Frequently
- Why Early Adaptation Is Important
- Practical Take-Home Messages
Age does not cause diabetes directly, but it slowly reduces your body’s ability to handle sugar
Many people notice that blood sugar becomes more difficult to control as they grow older, even without major lifestyle changes. Meals that were once well tolerated now lead to higher readings, and weight becomes harder to manage.
This is not just coincidence. Age-related changes in metabolism, hormones, and body composition make glucose control progressively more challenging.
Does Age Directly Increase Blood Sugar?
Age itself is not the direct cause of high blood sugar. The real issue is that several physiological processes change over time. These changes affect how the body produces, uses, and responds to insulin.
As a result, the same lifestyle that worked in younger years may no longer be sufficient to maintain metabolic balance.
Decline in Insulin Sensitivity
One of the most important changes with age is reduced insulin sensitivity. This means that body cells do not respond as effectively to insulin, making it harder for glucose to enter the cells.
To compensate, the body produces more insulin. Initially, this keeps blood sugar normal, but over time, this mechanism becomes inefficient and sugar levels start rising.
Loss of Muscle Mass (Sarcopenia)
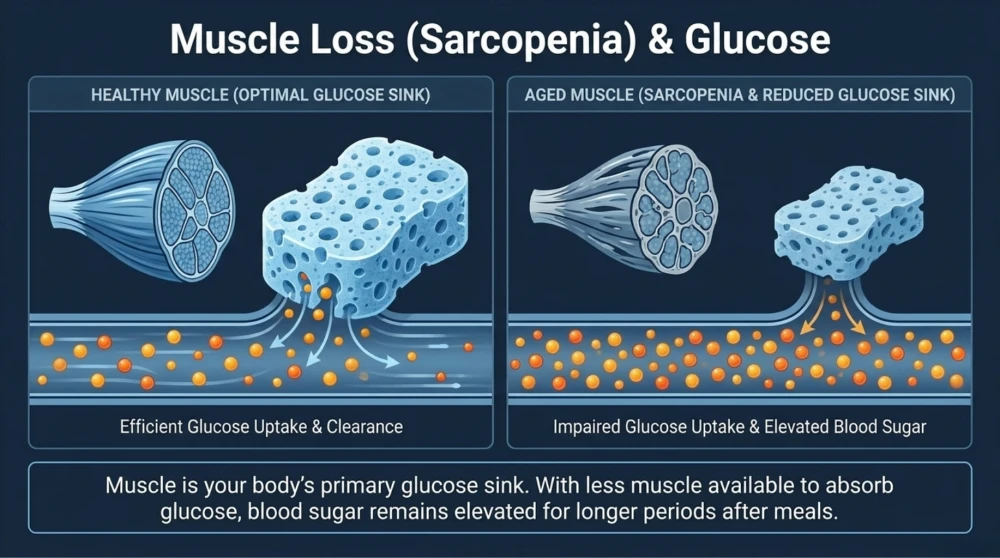
Muscle plays a major role in glucose utilization. As age increases, there is a gradual loss of muscle mass, a condition known as sarcopenia.
With less muscle available to absorb glucose, blood sugar remains elevated for longer periods after meals.
Increase in Abdominal Fat
Aging is often associated with an increase in visceral or abdominal fat. This type of fat is metabolically active and strongly linked with insulin resistance.
Even if overall body weight does not change significantly, a shift toward central fat distribution can worsen glucose control.
Changes in Hormonal Regulation
Hormonal balance also changes with age. Levels of growth hormone, testosterone, and estrogen decline, all of which play roles in metabolism and insulin sensitivity.
These changes contribute to reduced metabolic efficiency and increased risk of glucose imbalance.
Reduced Physical Activity and Its Impact
With increasing age, daily physical activity often reduces. Sedentary habits gradually replace earlier levels of movement, whether due to work patterns, joint issues, or lifestyle changes.
This reduction directly affects glucose utilization because muscles play a key role in absorbing glucose. When activity levels drop, glucose remains in the bloodstream longer, contributing to higher post-meal readings.
Slower Metabolic Rate
Basal metabolic rate naturally declines with age. This means the body burns fewer calories at rest, and excess energy is more likely to be stored as fat.
This shift not only promotes weight gain but also worsens insulin resistance, making blood sugar control more difficult even without major dietary changes.
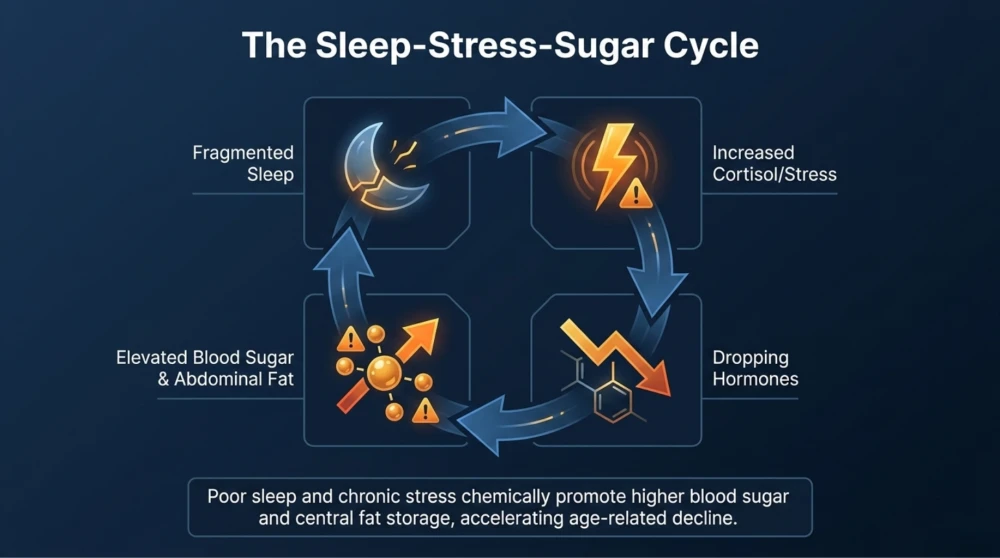
Impact of Sleep and Stress
Sleep patterns often change with age, and many individuals experience lighter or fragmented sleep. Poor sleep directly affects insulin sensitivity and increases stress hormone levels.
Chronic stress further elevates cortisol, which promotes higher blood sugar levels and increases abdominal fat accumulation.
Medication and Comorbid Conditions
As people age, the likelihood of other medical conditions increases. Medications for conditions such as hypertension, arthritis, or hormonal disorders can sometimes influence glucose metabolism.
Additionally, conditions like thyroid disorders or fatty liver can indirectly worsen blood sugar control.
Why Post-Meal Sugar Becomes More Important With Age
In older adults, post-meal spikes become more prominent due to reduced insulin response and decreased muscle mass. Even when fasting sugar appears acceptable, post-meal values may be significantly elevated.
This makes post-meal monitoring particularly important in this age group.
The Cumulative Effect Over Time
The challenge with age-related metabolic changes is that they develop gradually. Each factor, whether reduced activity, hormonal changes, or increased fat mass, contributes incrementally.
Over years, this cumulative effect significantly increases the risk of developing diabetes and related complications.

What Can You Do to Maintain Better Sugar Control With Age?
Although age-related changes cannot be completely avoided, their impact can be significantly reduced with the right approach. The focus should be on improving metabolic efficiency rather than simply reacting to rising sugar levels.
1. Preserve and Build Muscle Mass
Strength training becomes increasingly important with age. Maintaining muscle helps improve glucose utilization and insulin sensitivity. Even simple resistance exercises performed regularly can make a meaningful difference.
2. Focus on Meal Composition
Balanced meals that include protein, fiber, and healthy fats slow down glucose absorption and reduce post-meal spikes. Avoiding refined carbohydrates and sugary foods becomes more important as metabolic flexibility decreases.
3. Stay Consistent With Physical Activity
Regular movement, especially after meals, helps muscles absorb glucose effectively. Even light activities like walking after meals can improve blood sugar control.
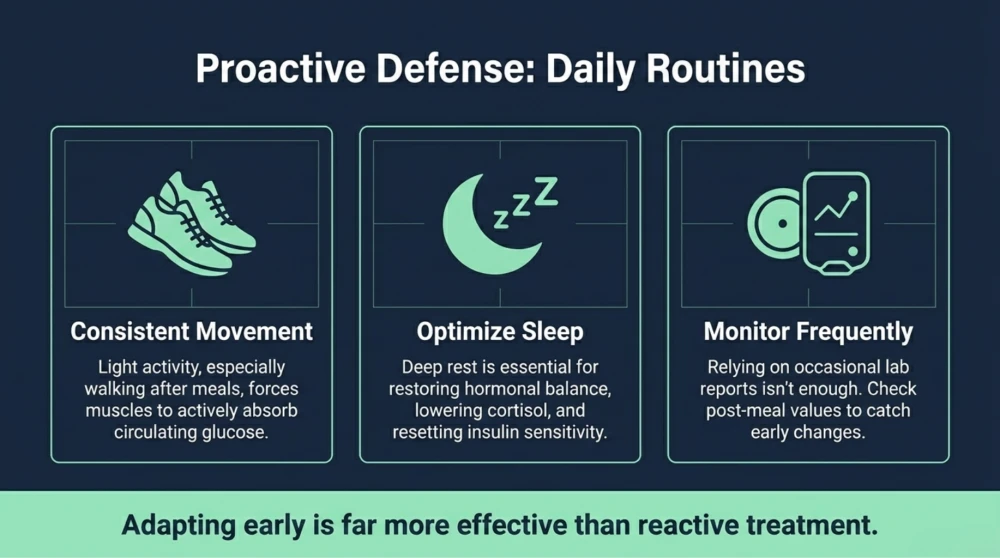
4. Improve Sleep Quality
Good sleep is essential for hormonal balance and insulin sensitivity. Addressing sleep issues can have a direct positive impact on glucose control.
5. Monitor More Frequently
As age increases, relying only on occasional lab reports may not be sufficient. Periodic monitoring, especially post-meal values, helps detect early changes and allows timely intervention.
Why Early Adaptation Is Important
Waiting for blood sugar to become abnormal makes management more difficult. Adapting lifestyle early helps slow down age-related metabolic decline and reduces long-term complications.
This proactive approach is far more effective than reactive treatment.
Practical Take-Home Messages
Blood sugar control becomes harder with age due to reduced insulin sensitivity, muscle loss, and changes in body composition. These changes are gradual but significant over time.
Maintaining muscle mass, staying active, and focusing on balanced nutrition can help counter these effects. Early and consistent intervention is the key to long-term metabolic health.
You can book a consultation here: Book Appointment
Written by Dr. Pankaj Kumar, General & Lifestyle Physician, Dwarka, New Delhi