
- 11th May 2026
Table of Contents
- “I Changed My Diet… So Why Is My Cholesterol Still High?”
- Cholesterol Is Not Just About Eating Fat
- The Liver Controls Most of the Cholesterol Metabolism
- Why Some Patients Improve Quickly While Others Do Not
- Insulin Resistance Quietly Changes Cholesterol Patterns
- Fatty Liver and Cholesterol Are Deeply Connected
- The “Healthy Eating but Poor Metabolism” Problem
- Why This Matters More Than Ever Today
- Why Weight Loss Alone Sometimes Fails to Normalize Cholesterol
- Visceral Fat Is More Dangerous Than Total Weight
- The Sedentary Lifestyle Problem Nobody Talks About Enough
- Sleep Is Quietly Affecting Cholesterol Too
- Stress Can Keep Cholesterol Elevated
- The “Healthy Processed Food” Trap
- Why Cholesterol Should Never Be Viewed in Isolation
- The Goal Should Be Metabolic Improvement, Not Just “Perfect Numbers”
- What Actually Works: A Smarter Approach to Cholesterol Improvement
- Focus on Insulin Sensitivity First
- Diet Quality Matters More Than Extreme Restriction
- Exercise Changes Cholesterol in Ways Diet Alone Cannot
- Sleep and Recovery Are Metabolic Therapies
- Sometimes Medication Is Still Necessary — And That Is Okay
- Why Extreme Dieting Usually Fails
- The Real Goal: Lower Cardiovascular Risk
- What I Commonly See in Clinical Practice
- Key Takeaways: What You Should Remember
- When Should You Seek Medical Evaluation?
Written by Dr. Pankaj Kumar, General & Lifestyle Physician, Dwarka, New Delhi
About Dr. Pankaj Kumar: https://www.dietplusminus.com/about-dr-pankaj-kumar
“I Changed My Diet… So Why Is My Cholesterol Still High?”
One of the most frustrating situations for many patients is seeing very little improvement in cholesterol levels despite making major dietary changes.
They stop fried foods. They reduce sweets. They avoid butter, ghee, and fast food. Some even lose weight. Yet when they repeat their blood tests after a few months, the cholesterol numbers still remain abnormal.
This often creates confusion, disappointment, and sometimes even guilt.
The most common reaction I hear in clinical practice is:
“Doctor, I followed the diet properly. Then why is my cholesterol still high?”
This is actually a very important question because it highlights one of the biggest misconceptions in metabolic health — the belief that cholesterol problems are caused only by food.
In reality, cholesterol metabolism is much more complicated than simply eating oily food.
Yes, diet matters. In fact, it matters a lot. But cholesterol regulation is influenced by multiple systems inside the body, including liver function, insulin sensitivity, hormonal balance, genetics, body fat distribution, physical activity, sleep quality, and even stress levels.
This is why two people can follow almost the same diet and still have completely different cholesterol profiles.
One person may improve dramatically with dietary correction alone, while another may continue struggling despite strict discipline.
Understanding this difference is extremely important because otherwise patients either become discouraged or start following extreme and unsustainable diets that eventually damage their overall metabolic health.
Cholesterol Is Not Just About Eating Fat
Most people think cholesterol comes directly from the food they eat. But the body itself produces cholesterol naturally because cholesterol is essential for survival.
Your liver continuously manufactures cholesterol because the body needs it for several critical functions:
- Hormone production
- Cell membrane structure
- Vitamin D synthesis
- Brain and nerve function
This means cholesterol is not simply a “bad substance.” It is actually a necessary biological component.
The real issue is not cholesterol alone, but how cholesterol is being processed, transported, and regulated inside the body.
And this regulation depends on the overall metabolic environment.
That is where things become complicated.
The Liver Controls Most of the Cholesterol Metabolism
The liver acts as the central processing unit for fat metabolism.
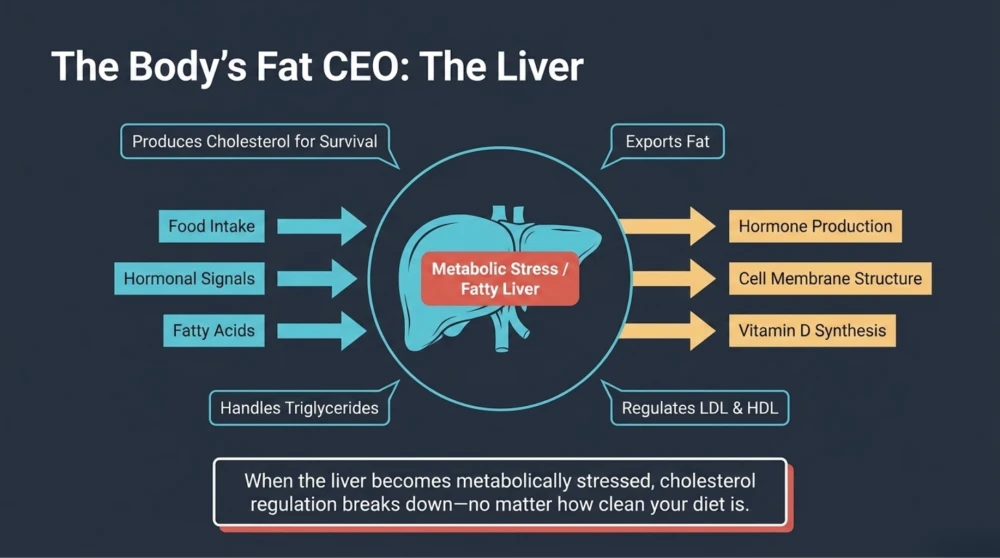
It decides:
- How much cholesterol to produce
- How much fat to export
- How triglycerides are handled
- How LDL and HDL particles behave
Now imagine what happens when the liver itself becomes metabolically unhealthy.
This is exactly what occurs in modern metabolic disorders like fatty liver and insulin resistance.
Many patients focus only on reducing dietary fat while the liver continues operating in a stressed and dysfunctional metabolic state.
This is why cholesterol abnormalities sometimes persist despite “healthy eating.”
Why Some Patients Improve Quickly While Others Do Not
One of the biggest reasons patients become confused is because cholesterol improvement is highly individual.
Some people respond extremely well to dietary changes. Within a few months, their triglycerides improve, HDL increases, and LDL levels reduce significantly.
But other patients notice only mild improvement. This difference usually depends on deeper metabolic factors.
For example, if someone has underlying insulin resistance, visceral fat accumulation, poor sleep, chronic stress, or fatty liver, then simply reducing oily food may not be enough to completely normalize cholesterol metabolism.
The body is still functioning in an unhealthy metabolic environment. This is why cholesterol should never be viewed in isolation.
Insulin Resistance Quietly Changes Cholesterol Patterns
One of the most overlooked reasons diet alone sometimes cannot correct cholesterol is insulin resistance.
Many people associate insulin resistance only with diabetes, but its effects begin much earlier.
Long before blood sugar becomes abnormal, insulin resistance starts affecting how the body handles fat.
In this state:
- The liver starts producing more triglycerides
- HDL cholesterol often decreases
- LDL particles become smaller and more harmful
This creates a pattern known as “atherogenic dyslipidemia,” which is very common in modern metabolic disease.
And importantly, this pattern may continue even if dietary fat intake is reduced.
This is why patients sometimes feel confused:
“I stopped oily food completely, but triglycerides are still high.”
The reason is that the body itself is now overproducing fat due to metabolic dysfunction. In other words, the issue is no longer only external food intake. The internal metabolic machinery has changed.
Fatty Liver and Cholesterol Are Deeply Connected
Another major reason cholesterol may remain abnormal despite dietary correction is fatty liver.
Most patients do not realize how closely the liver and cholesterol metabolism are connected.
When fat starts accumulating inside liver cells, the liver becomes less efficient at regulating fat transport and storage.
This affects:
- Triglyceride production
- LDL regulation
- Fat oxidation
- Insulin sensitivity
This is why patients with fatty liver frequently show persistent triglyceride elevation and low HDL cholesterol.
And this also explains why improving only food quality without correcting overall metabolism may not produce dramatic results.
The “Healthy Eating but Poor Metabolism” Problem
One of the most important clinical observations today is this: Many individuals are eating “healthier” than before, but their metabolism is still unhealthy.
Why?
Because metabolism is influenced not just by food quality but also by:
- Sleep timing
- Stress exposure
- Physical activity
- Muscle mass
- Sedentary behavior
This is why a patient may avoid junk food yet still struggle with:
- High triglycerides
- Low HDL
- Borderline LDL abnormalities
- Fatty liver
The modern metabolic environment itself is contributing to the problem.
Why This Matters More Than Ever Today
Modern lifestyle has changed dramatically over the last two decades.
Today many people:
- Sit for prolonged hours
- Sleep late
- Experience chronic stress
- Eat frequently throughout the day
- Have low muscle activity
All these factors influence cholesterol metabolism.
This is why cholesterol management today requires a much broader and more intelligent approach than simply saying “avoid oily food.”
This is also why structured metabolic approaches like the Lifestyle Modification Program focus on the entire metabolic ecosystem rather than only dietary fat restriction.
Why Weight Loss Alone Sometimes Fails to Normalize Cholesterol
Another reason many patients become discouraged is because they expect cholesterol to improve automatically after weight loss.
And to be fair, this expectation is not completely wrong. In many cases, losing excess body fat does improve triglycerides, HDL cholesterol, insulin sensitivity, and overall cardiovascular risk.
But the relationship between weight loss and cholesterol is not always linear.
Some patients lose significant weight and still notice persistent lipid abnormalities. Others lose only a few kilograms and see dramatic improvement.
This difference happens because body weight alone does not accurately reflect metabolic health.
What matters more is:
- Where fat is stored
- How the liver is functioning
- How insulin-sensitive the body is
- How much muscle mass is present
This is why two individuals with the same body weight can have completely different cholesterol profiles.
Visceral Fat Is More Dangerous Than Total Weight
One of the biggest metabolic problems today is excess visceral fat.
This is the fat stored around internal organs, especially around the liver and abdomen.
Unlike subcutaneous fat under the skin, visceral fat is metabolically active. It constantly releases inflammatory chemicals and fatty acids into the bloodstream.
This creates a situation where:
- The liver receives excess fat continuously
- Triglyceride production increases
- Insulin resistance worsens
- HDL cholesterol often decreases
This explains why some individuals with moderate weight still have severe metabolic abnormalities.
It also explains why simply reducing calories without improving body composition may not completely normalize cholesterol metabolism.
The Sedentary Lifestyle Problem Nobody Talks About Enough
One of the biggest reasons cholesterol remains abnormal despite dietary changes is physical inactivity.
Modern life has dramatically reduced daily movement.
Many people now spend most of the day:
- Sitting at desks
- Using screens
- Driving or commuting
- Remaining physically inactive for long hours
This changes metabolism in ways that most people do not realize.
When muscles remain inactive for prolonged periods:
- Fat oxidation decreases
- Insulin sensitivity worsens
- Triglycerides tend to rise
- HDL cholesterol often falls
This means a patient can technically “eat healthy” while still living in a metabolically unhealthy state.
That is why exercise is not simply about burning calories. Physical activity directly improves how the body handles fats and carbohydrates.
This is also why cholesterol correction usually becomes much more effective when proper movement and resistance training are added.
Sleep Is Quietly Affecting Cholesterol Too
Many patients never connect sleep with cholesterol levels. But poor sleep significantly affects metabolic regulation.
Inadequate sleep changes:
- Hormonal balance
- Appetite regulation
- Insulin sensitivity
- Stress hormone levels
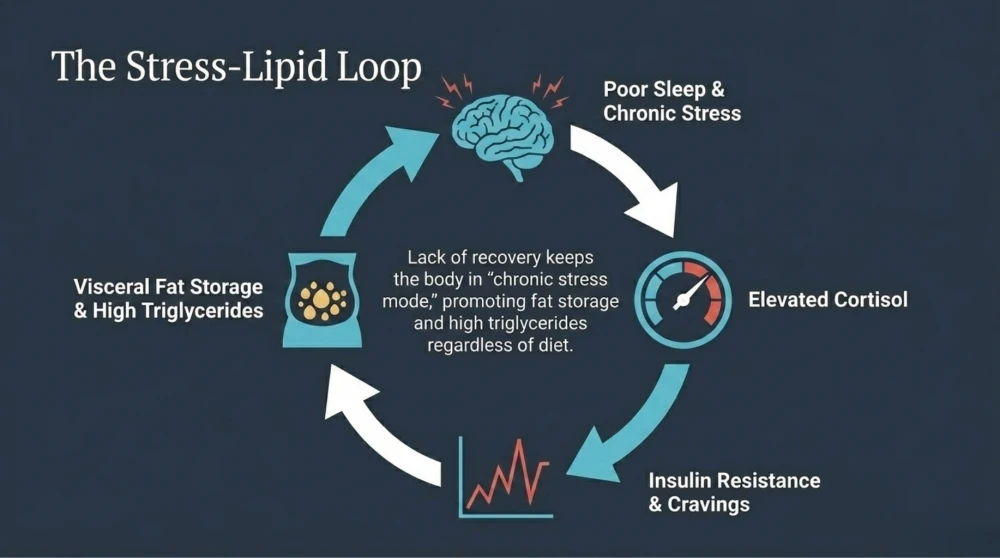
When sleep quality deteriorates, cortisol levels remain elevated for longer durations.
This promotes:
- Fat storage
- Increased cravings
- Poor glucose regulation
- Higher triglycerides
This is why patients who sleep late, work irregular schedules, or experience chronic sleep deprivation often struggle with persistent metabolic abnormalities despite improving diet quality.
Stress Can Keep Cholesterol Elevated
Chronic stress is another underestimated factor. Modern lifestyles have created continuous low-grade psychological stress for many individuals.
Financial pressure, work deadlines, screen overload, lack of recovery, and poor work-life balance all affect metabolic physiology.
When stress becomes chronic:
- Cortisol levels remain elevated
- Inflammation increases
- Insulin resistance worsens
- Visceral fat accumulation increases
This directly affects lipid metabolism.
In clinical practice, many patients notice cholesterol improvement only after improving overall lifestyle rhythm — not just food.
The “Healthy Processed Food” Trap
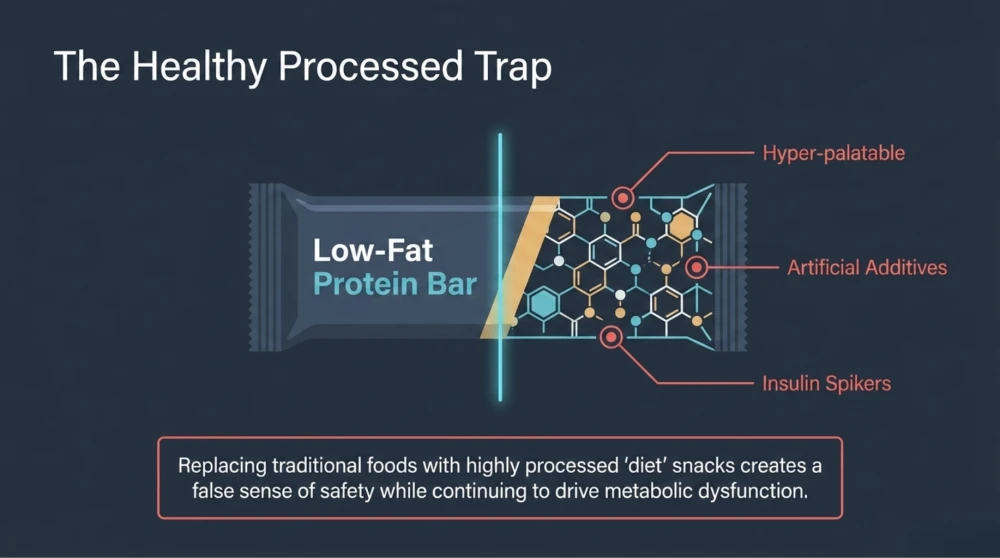
One of the most interesting modern problems is the rise of ultra-processed “healthy” foods.
Many individuals replace traditional foods with:
- Diet snacks
- Low-fat packaged products
- Protein bars
- Sugar-free processed foods
These products often create a false sense of metabolic safety.
But many are still:
- Highly processed
- Rich in additives
- Artificially flavored
- Designed for hyper-palatability
This can continue promoting overeating, insulin spikes, and metabolic dysfunction. So even though the label appears “healthy,” the metabolic impact may still be problematic.
Why Cholesterol Should Never Be Viewed in Isolation
One of the biggest mistakes in modern healthcare is focusing only on isolated cholesterol numbers.
Cholesterol is deeply connected with:
- Insulin resistance
- Fatty liver
- Body composition
- Inflammation
- Metabolic flexibility
This means lipid abnormalities are often part of a much larger metabolic picture. That is why patients who only focus on reducing oily food frequently become frustrated.
The real solution usually requires improving the entire metabolic environment.
The Goal Should Be Metabolic Improvement, Not Just “Perfect Numbers”
Another important concept patients need to understand is this: Health is not determined by one isolated number.
Sometimes cholesterol improves only modestly, but the patient experiences major improvement in:
- Energy levels
- Waist circumference
- Blood sugar control
- Liver health
- Physical fitness
These changes are still extremely valuable.
This is why long-term cardiovascular risk reduction matters more than chasing perfection in one lab report.
What Actually Works: A Smarter Approach to Cholesterol Improvement
Once patients understand that diet alone sometimes cannot correct cholesterol, the next question naturally becomes:
“Then what should I actually focus on?”
The answer is surprisingly simple — stop looking at cholesterol as an isolated food problem and start looking at it as a metabolic health issue.
This single shift in understanding changes everything.
Because when cholesterol abnormalities are viewed only through the lens of dietary fat, patients often end up following extremely restrictive and unsustainable eating patterns.

They become afraid of:
- Traditional foods
- Healthy fats
- Social eating
- Normal meals
Meanwhile, the real metabolic drivers continue silently in the background.
This is why cholesterol management should always focus on improving the overall metabolic environment.
Focus on Insulin Sensitivity First
One of the most powerful ways to improve cholesterol naturally is by improving insulin sensitivity.
When insulin sensitivity improves:
- Triglycerides often reduce
- HDL cholesterol may improve
- Fatty liver starts reversing
- Inflammation decreases
This is why many patients see dramatic lipid improvement not by “removing fat,” but by correcting carbohydrate overload, reducing visceral fat, improving activity levels, and stabilizing metabolism.
In fact, some patients become frustrated because they are eating “low-fat” diets while still consuming excessive refined carbohydrates.
This often keeps triglycerides elevated.
That is why improving metabolic flexibility matters more than blindly eliminating fats.
Diet Quality Matters More Than Extreme Restriction
Many individuals believe cholesterol correction requires severe dietary restriction. But in reality, sustainability matters much more than temporary perfection.
The goal should not be starvation or fear-based eating. The goal should be reducing the foods that continuously overload the metabolic system.
In clinical practice, I usually focus on:
- Reducing refined carbohydrates
- Controlling sugar intake
- Improving protein intake
- Increasing fiber-rich foods
- Minimizing ultra-processed foods
These changes improve the body’s ability to regulate fats naturally.
And importantly, they are sustainable long term.
Exercise Changes Cholesterol in Ways Diet Alone Cannot
This is one of the biggest reasons why some patients see only partial improvement with dietary correction alone.
Physical activity affects cholesterol metabolism directly.
Regular movement improves:
- HDL cholesterol levels
- Fat oxidation
- Insulin sensitivity
- Mitochondrial function
Resistance training is especially important because muscle tissue acts like a major metabolic engine.
More muscle activity means:
- Better glucose handling
- Improved fat utilization
- Reduced triglyceride production
This is why many patients notice a much bigger improvement once exercise becomes consistent.
Sleep and Recovery Are Metabolic Therapies
Modern healthcare still underestimates the importance of recovery.
Patients are often told what to eat but rarely taught how deeply sleep affects metabolism. Poor sleep keeps the body in a stressed physiological state.
This affects:
- Appetite regulation
- Insulin sensitivity
- Fat metabolism
- Stress hormone balance
In many individuals, improving sleep quality alone creates noticeable metabolic improvement.
This is why sustainable cholesterol correction requires:
- Consistent sleep timing
- Reduced late-night stimulation
- Better recovery patterns
These changes help the body shift from chronic stress mode into metabolic repair mode.
Sometimes Medication Is Still Necessary — And That Is Okay
This is another important conversation many patients struggle with emotionally.
Some people believe needing medication means they “failed” at lifestyle management. That is simply not true.
If strong genetic factors, severe insulin resistance, advanced metabolic disease, or long-standing cholesterol abnormalities are present, medication may still be necessary even with excellent lifestyle habits.
But this does not reduce the importance of lifestyle correction.
In fact, medications work far more effectively when combined with:
- Proper diet
- Exercise
- Weight reduction
- Better sleep
- Stress management
The best outcomes usually come from combining both approaches intelligently.
Why Extreme Dieting Usually Fails
One of the biggest mistakes patients make is trying aggressive short-term diets.
They follow highly restrictive eating plans for a few weeks, see temporary improvement, and then eventually return to old habits.
This creates a cycle of:
- Restriction
- Frustration
- Rebound eating
- Metabolic instability
Long-term consistency always beats short-term intensity.
This is why sustainable cholesterol correction requires building a lifestyle that can realistically continue for years.
The Real Goal: Lower Cardiovascular Risk
Patients often become obsessed with achieving “perfect” cholesterol numbers. But the real goal is much bigger.
The actual objective is reducing long-term cardiovascular risk and improving metabolic health.
This includes:
- Reducing visceral fat
- Improving insulin sensitivity
- Lowering inflammation
- Protecting blood vessels
- Supporting liver health
When these systems improve together, cholesterol regulation usually improves much more naturally.
What I Commonly See in Clinical Practice
Many patients initially focus only on food restriction.
But the patients who improve most consistently are usually the ones who:
- Improve overall lifestyle rhythm
- Become physically active
- Sleep better
- Reduce chronic stress
- Build sustainable eating patterns
Over time, they often notice improvement not just in cholesterol, but also in:
- Energy levels
- Body composition
- Fatty liver
- Blood sugar control
- Overall metabolic health
This is why structured metabolic programs work better than isolated dietary restriction.
You can explore this broader approach through the Lifestyle Modification Program.
Key Takeaways: What You Should Remember
- Diet is important, but cholesterol metabolism is influenced by many other factors
- Insulin resistance and fatty liver play major roles in persistent lipid abnormalities
- Physical inactivity, stress, and poor sleep can worsen cholesterol despite healthy eating
- Genetics strongly influence how individuals respond to dietary changes
- The goal should be improving metabolic health, not just chasing one lab number
- Sustainable lifestyle correction works better than extreme restriction
- Medication may sometimes still be necessary, and that does not mean failure
When Should You Seek Medical Evaluation?
You should consider professional evaluation if you have:
- Persistently abnormal cholesterol reports
- High triglycerides
- Fatty liver
- Strong family history of heart disease
- Increasing belly fat or insulin resistance
Early intervention can significantly reduce long-term cardiovascular risk.
You can book a consultation here:
Book Appointment









.webp)




