- 17th April 2026
Table of Contents
- Your fasting sugar may look fine, but your post-meal spike decides your future risk
- What Exactly Is Post-Meal Blood Sugar?
- Why Post-Meal Sugar Becomes Abnormal First
- The Silent Damage Caused by Post-Meal Spikes
- Why HbA1c Alone Can Be Misleading
- Clinical Insight
- Why Post-Meal Spikes Matter More Than Fasting Sugar
- The Role of Insulin in Post-Meal Control
- Glycemic Variability: The Hidden Risk Factor
- Common Triggers of Post-Meal Spikes
- Evening Meals and Late-Night Snacking
- Why Symptoms Often Appear After Meals
- What Should You Do to Control Post-Meal Sugar?
- 1. Balance Your Meals
- 2. Improve Meal Timing
- 3. Stay Physically Active After Meals
- 4. Focus on Food Quality
- 5. Monitor When Needed
- Why Early Control Is Important
- Practical Take-Home Messages
Your fasting sugar may look fine, but your post-meal spike decides your future risk
In clinical practice, I often see patients who are reassured because their fasting blood sugar or HbA1c (glycated haemoglobin) is normal. However, they still complain of fatigue, sleepiness after meals, or difficulty controlling weight. This is where post-meal sugar becomes extremely important.
Post-meal blood sugar is usually the first parameter to become abnormal in metabolic dysfunction. Ignoring it delays early diagnosis and allows silent damage to continue.
What Exactly Is Post-Meal Blood Sugar?
Post-meal (postprandial) blood sugar reflects how efficiently your body handles glucose after eating. After a meal, glucose levels rise and insulin is released to push that glucose into cells. In a healthy system, this rise is controlled and returns to baseline within a few hours.
But when insulin response is delayed or ineffective, glucose remains elevated for longer. This prolonged elevation is what gradually disturbs metabolism.
Why Post-Meal Sugar Becomes Abnormal First
In early stages of metabolic dysfunction, the body can still maintain normal fasting sugar by compensating with higher insulin levels. However, this compensation is not efficient during meals, where a sudden glucose load is present.
As a result, post-meal spikes appear much earlier than fasting abnormalities. This is why many patients with “normal reports” are already metabolically unhealthy.
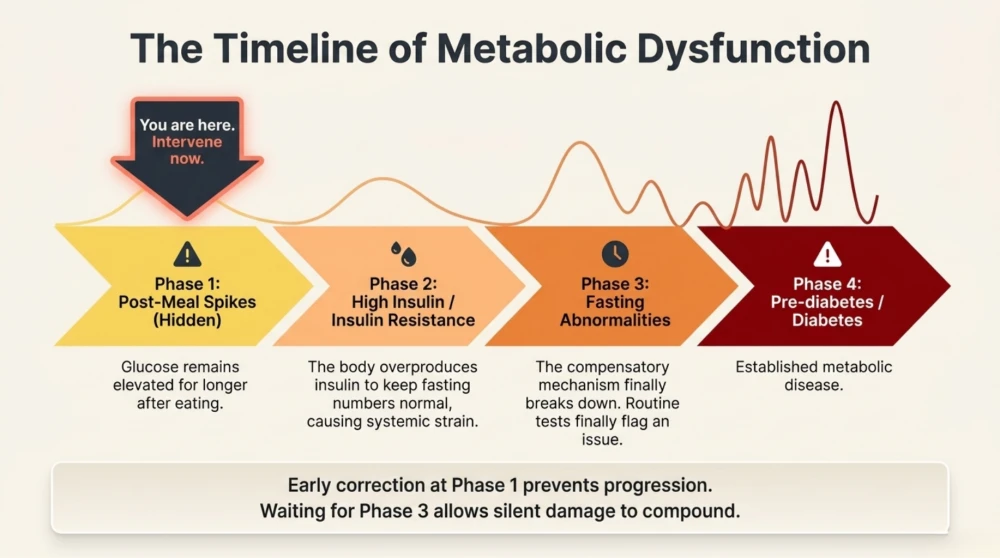
The Silent Damage Caused by Post-Meal Spikes
Repeated post-meal spikes are not harmless. They trigger oxidative stress and low-grade inflammation, which slowly damage blood vessels and metabolic pathways. Over time, this contributes to conditions like diabetes, fatty liver, and cardiovascular disease.
The important point is that this damage begins long before fasting sugar becomes abnormal.
Why HbA1c Alone Can Be Misleading
HbA1c reflects the average blood sugar over the past two to three months, but it does not capture fluctuations. A person can have normal HbA1c yet experience frequent high spikes after meals.
This means the average looks acceptable, but the body is still exposed to repeated metabolic stress throughout the day.
Clinical Insight
It is not uncommon to see patients with normal fasting sugar and HbA1c but significantly elevated post-meal values. These patients often present with early symptoms like fatigue, cravings, and central weight gain.
This stage is critical because intervention at this point can prevent progression to diabetes.
Why Post-Meal Spikes Matter More Than Fasting Sugar
Fasting sugar reflects your baseline metabolism after several hours without food. It is a stable number and often remains normal for a long time, even when underlying dysfunction has already started. In contrast, post-meal sugar tests your system under stress.
When you eat, especially carbohydrates, your body must quickly regulate rising glucose. If this response is inefficient, it clearly indicates early metabolic imbalance. This is why post-meal readings often reveal problems earlier than fasting values.
The Role of Insulin in Post-Meal Control
Insulin plays a central role in controlling post-meal sugar. In early insulin resistance, the body produces more insulin to keep fasting sugar normal, but this mechanism becomes inadequate during meals when glucose load increases suddenly.
This leads to higher spikes and delayed return to normal levels. Over time, this strain on the system worsens insulin resistance further.
Glycemic Variability: The Hidden Risk Factor
Even if your average sugar is normal, large fluctuations throughout the day can be harmful. This is known as glycemic variability, and it is increasingly recognized as an independent risk factor for metabolic disease.
Frequent spikes followed by drops can lead to fatigue, irritability, and increased hunger. These fluctuations also contribute to long-term complications.
Common Triggers of Post-Meal Spikes
Post-meal spikes are strongly influenced by daily habits. Refined carbohydrates, sugary beverages, and large portion sizes can cause rapid glucose elevation. Eating quickly or consuming meals without protein or fiber further worsens the response.
Lifestyle factors like poor sleep, stress, and sedentary behavior also reduce the body’s ability to handle glucose efficiently.
Evening Meals and Late-Night Snacking
The timing of meals also matters. In the evening, insulin sensitivity naturally decreases. This means the same meal can produce a higher spike at night compared to daytime.
Late-night snacking adds repeated glucose load when the body is least prepared to handle it, leading to prolonged elevation and fat storage.

Why Symptoms Often Appear After Meals
Many patients notice symptoms specifically after eating. This includes sleepiness, lack of energy, or sudden cravings within a few hours. These are often linked to rapid rise and fall in blood sugar levels.
Such symptoms are early indicators that the body is struggling to maintain stable glucose levels.
What Should You Do to Control Post-Meal Sugar?
The goal is not just to keep sugar “within range,” but to prevent sharp spikes after meals. This requires a combination of meal planning, timing, and lifestyle correction rather than relying only on medication.
1. Balance Your Meals
Meals that include protein, fiber, and healthy fats slow down glucose absorption. Instead of eating carbohydrates alone, combining them with protein sources like paneer, eggs, or dal helps reduce post-meal spikes significantly.
2. Improve Meal Timing
Spacing meals properly and avoiding frequent snacking allows insulin levels to stabilize. Late-night eating should be minimized because the body’s glucose-handling capacity is lower in the evening.
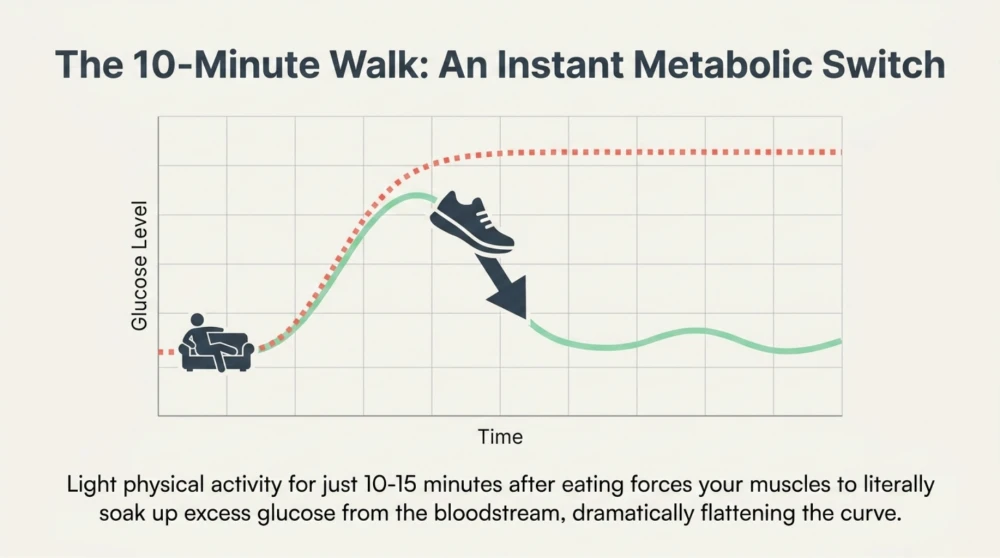
3. Stay Physically Active After Meals
Even light activity like walking for 10–15 minutes after meals can improve glucose uptake by muscles. This simple habit can reduce post-meal spikes effectively.
4. Focus on Food Quality
Highly refined foods and sugary beverages cause rapid glucose elevation. Replacing them with whole foods, complex carbohydrates, and fiber-rich options improves metabolic response.
5. Monitor When Needed
If there is concern about post-meal spikes, targeted monitoring can provide clarity. Checking sugar 1–2 hours after meals or using continuous glucose monitoring (CGM) helps identify patterns.
Why Early Control Is Important
Post-meal spikes are often the first sign of metabolic dysfunction. If ignored, they gradually progress to sustained high blood sugar, leading to diabetes and related complications.
Early correction at this stage is much easier and more effective than managing established disease later.
Practical Take-Home Messages
Post-meal sugar is one of the earliest indicators of metabolic imbalance. Even when fasting sugar and HbA1c are normal, repeated spikes can silently damage metabolism.
Simple lifestyle changes such as balanced meals, proper timing, and post-meal activity can significantly improve glucose control and prevent long-term disease.
You can book a consultation here: Book Appointment
Written by Dr. Pankaj Kumar, General & Lifestyle Physician, Dwarka, New Delhi