- 15th April 2026
Table of Contents
- Normal reports do not always mean normal metabolism
- What “Normal Blood Sugar” Actually Means
- The Hidden Phase: Early Metabolic Dysfunction
- Common Symptoms Despite Normal Sugar Levels
- Why Standard Tests May Miss the Problem
- The Role of Insulin: The Missing Piece in Most Reports
- Post-Meal Spikes: The Hidden Fluctuations
- The Concept of Glycemic Variability
- Why HbA1c May Be Misleading in Early Stages
- The Role of Lifestyle in These Symptoms
- When Should You Suspect a Hidden Problem?
- What Should You Do If You Have Symptoms but Normal Reports?
- Why Early Action Matters
- Practical Take-Home Messages
- References
Written by Dr. Pankaj Kumar, General & Lifestyle Physician, Dwarka, New Delhi
About Dr. Pankaj Kumar: https://www.dietplusminus.com/about-dr-pankaj-kumar
Normal reports do not always mean normal metabolism
Many patients come with a common concern: their blood sugar reports are within normal range, yet they experience symptoms like fatigue, cravings, brain fog, or sudden weakness.
This creates confusion. If reports are normal, why do symptoms persist? The answer lies in understanding that blood sugar levels alone do not reflect complete metabolic health.
What “Normal Blood Sugar” Actually Means
Standard reports typically include fasting blood sugar, post-meal blood sugar, and HbA1c (glycated haemoglobin). These values fall within a defined range considered “normal.”
However, these tests provide snapshot information, do not show daily fluctuations, and do not reflect early metabolic dysfunction. This is where many early problems remain undetected.
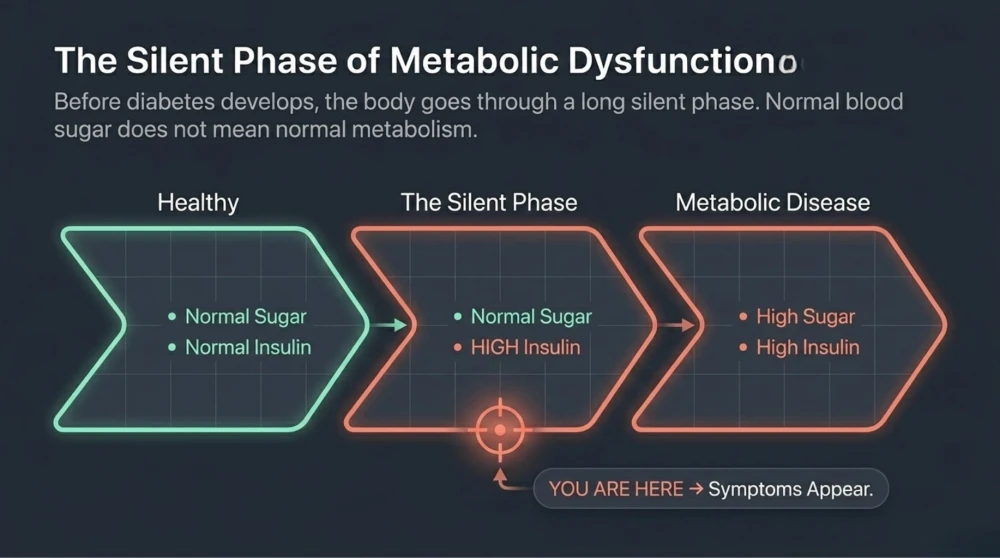
The Hidden Phase: Early Metabolic Dysfunction
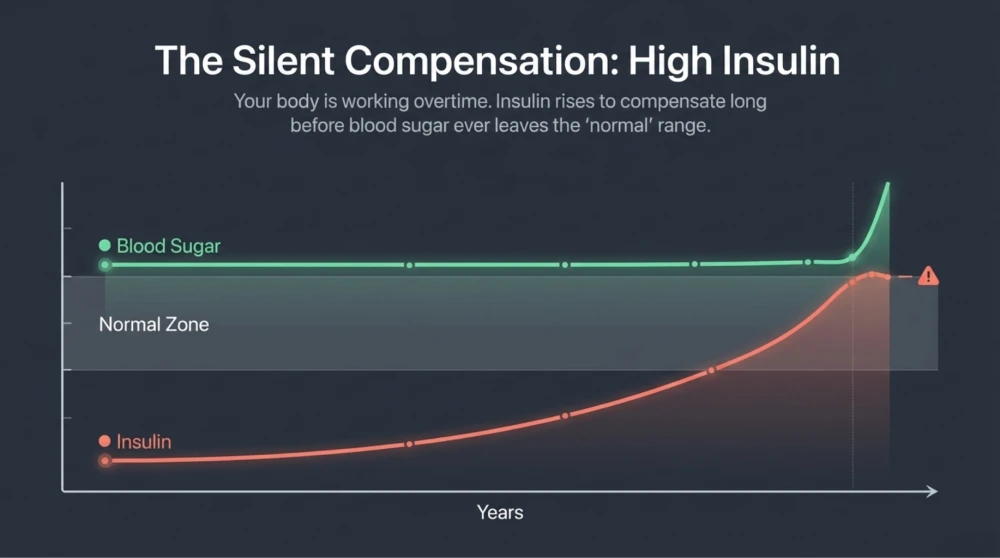
Before diabetes develops, the body goes through a long silent phase. During this stage insulin levels rise, cells become resistant to insulin, and blood sugar may still remain “normal”. This condition is called insulin resistance.
It is one of the most common reasons why patients feel symptoms despite normal reports.
Common Symptoms Despite Normal Sugar Levels
- Persistent fatigue
- Frequent hunger or cravings
- Sleepiness after meals
- Difficulty concentrating
- Weight gain, especially abdominal
These symptoms indicate metabolic imbalance, not necessarily overt diabetes.
Why Standard Tests May Miss the Problem
Routine tests are designed to diagnose disease, not detect early dysfunction. For example:
- Fasting sugar may be normal even with high insulin
- HbA1c reflects average, not fluctuations
- Post-meal spikes may go unnoticed
This is why patients can feel symptoms even when reports appear reassuring.
The Role of Insulin: The Missing Piece in Most Reports
Most routine reports measure glucose, but very few assess insulin levels. Insulin is the hormone responsible for moving glucose from the bloodstream into cells. In early metabolic dysfunction:
- Insulin levels increase to compensate
- Blood sugar remains normal temporarily
- Underlying imbalance continues to worsen
This means your body is working harder to maintain “normal” numbers. Over time, this compensation fails, and blood sugar starts rising.
Post-Meal Spikes: The Hidden Fluctuations
Many patients experience sharp rises and falls in blood sugar after meals, even when fasting values are normal. These fluctuations can cause energy crashes, sudden hunger, and irritability.
Standard tests often miss these spikes because they are not continuous measurements.
The Concept of Glycemic Variability
Even if average sugar levels are normal, wide fluctuations can still affect health. This is known as glycemic variability.
High variability is associated with:
- Increased oxidative stress
- Early metabolic dysfunction
- Higher long-term risk of diabetes
This explains why symptoms can exist without abnormal reports.
Why HbA1c May Be Misleading in Early Stages
HbA1c (glycated haemoglobin) reflects average blood sugar over 2–3 months. However:
- It does not show spikes
- It does not show insulin levels
- It may appear normal despite early dysfunction
This is why relying only on HbA1c can miss early warning signs.
The Role of Lifestyle in These Symptoms
Lifestyle patterns play a major role in this mismatch between reports and symptoms.
- Frequent snacking
- Sedentary behavior
- Poor sleep
- High stress
These factors gradually impair metabolic efficiency without immediately affecting blood sugar levels.
Contact here for personalised lifestyle modification program.
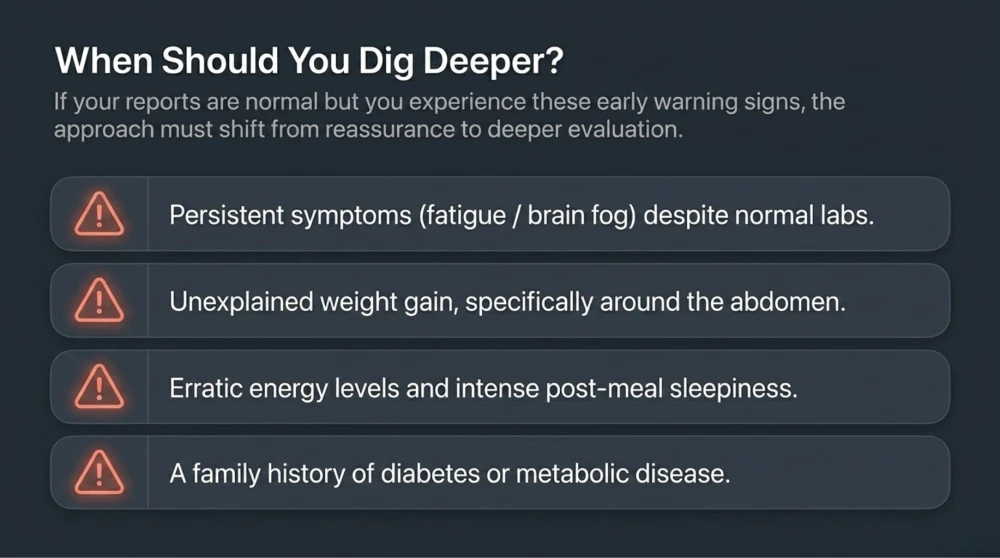
When Should You Suspect a Hidden Problem?
You should consider deeper evaluation if symptoms persist despite normal reports, or there is family history of diabetes, or unexplained weight gain or there is significant fluctuation in energy levels.
These are early warning signs that should not be ignored.
What Should You Do If You Have Symptoms but Normal Reports?
If your reports are normal but symptoms persist, the approach should shift from reassurance to deeper evaluation.
Instead of ignoring symptoms, focus on identifying early metabolic changes.
1. Look Beyond Basic Tests
Additional assessments may help:
- Fasting insulin levels
- HOMA-IR (insulin resistance index)
- Continuous glucose monitoring (CGM)
These tests provide better insight into metabolic function than glucose alone.
2. Focus on Lifestyle Correction
Even without abnormal reports, correcting lifestyle can significantly improve symptoms.
- Reduce frequent snacking
- Improve meal timing
- Increase physical activity
- Prioritize sleep
These changes target the root cause rather than waiting for disease to develop.
3. Monitor Patterns, Not Just Numbers
Instead of focusing only on lab values, observe:
- Energy levels
- Hunger patterns
- Sleep quality
These are early indicators of metabolic health.
Why Early Action Matters
Metabolic diseases develop gradually. By the time reports become abnormal:
- Damage has already progressed
- Reversal becomes more difficult
Early intervention provides:
- Higher chance of reversal
- Better long-term outcomes
- Reduced dependence on medication
Practical Take-Home Messages
- Normal blood sugar reports do not always mean normal metabolic health
- Symptoms can appear before lab abnormalities
- Insulin resistance often develops silently
- Glycemic variability plays an important role
- Early lifestyle correction can prevent disease progression